How to Know If Tooth Infection Spread to Brain Guide
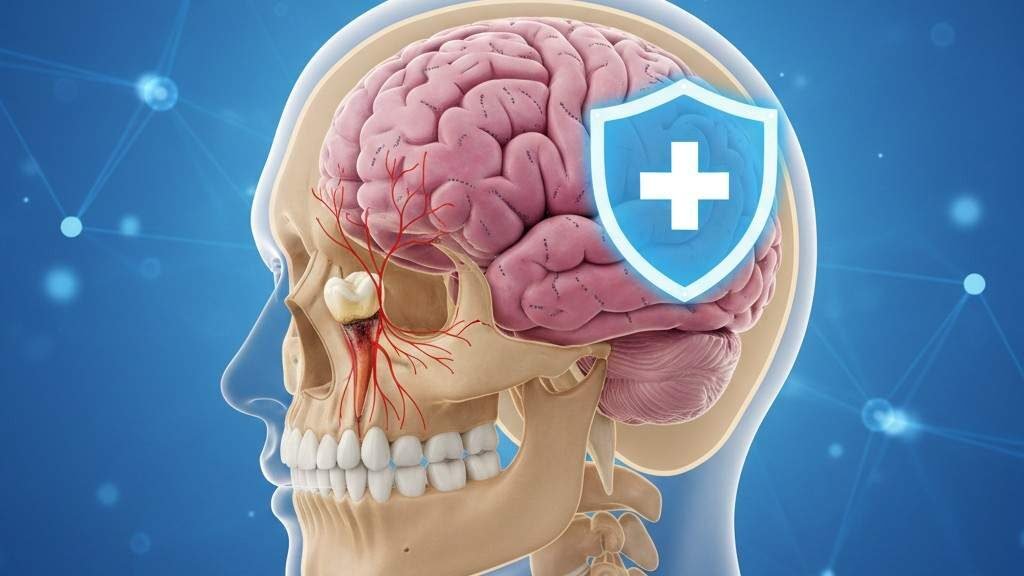
A toothache is never pleasant—but sometimes it can signal something far more serious. Many people search for how to know if tooth infection spread to brain because they’re worried about severe symptoms that go beyond normal dental pain. While this complication is rare, it can be life-threatening if ignored.
Dental infections usually stay localized in the tooth or gums. However, in untreated cases, bacteria can travel through surrounding tissues, blood vessels, or sinuses. Recognizing the early and advanced warning signs can help you act quickly and prevent serious outcomes.
This expert guide explains the real symptoms, medical risks, diagnosis process, treatment options, and when you should seek emergency care in the United States.
How Tooth Infections Spread
A tooth infection (also called a dental abscess) occurs when bacteria enter the pulp of the tooth. This often happens due to:
- Deep cavities
- Cracked or broken teeth
- Untreated gum disease
- Failed dental work
If left untreated, bacteria multiply and form pus. The infection can then spread to:
- Jawbone
- Neck tissues
- Sinuses
- Bloodstream
- Brain (in rare but severe cases)
The brain is protected by the skull and blood-brain barrier, but aggressive infections can sometimes bypass these defenses.
Why Brain Spread Is Dangerous
When bacteria reach the brain, they can cause:
- Brain abscess
- Meningitis
- Sepsis
- Cavernous sinus thrombosis
These are medical emergencies requiring immediate hospitalization.
Understanding how to know if tooth infection spread to brain starts with recognizing that symptoms go far beyond typical dental pain.
Early Warning Signs of a Severe Dental Infection
Before an infection reaches the brain, it often causes systemic symptoms. Watch for:
H3: Persistent High Fever
A fever above 101°F that doesn’t improve may indicate the infection is spreading.
H3: Facial Swelling That Worsens
Swelling extending to the eye, neck, or cheek is concerning.
H3: Severe Throbbing Pain
Pain that radiates to the ear, temple, or jaw may signal deeper involvement.
H3: Difficulty Swallowing or Breathing
This may suggest the infection is spreading into neck tissues.
If these symptoms appear, seek urgent dental or medical care immediately.
Advanced Symptoms: Possible Brain Involvement
If you’re wondering how to know if tooth infection spread to brain, these neurological signs are red flags:
- Severe headache different from normal headaches
- Confusion or disorientation
- Sensitivity to light
- Seizures
- Vision changes
- Neck stiffness
- Persistent vomiting
- Slurred speech
These symptoms require emergency room evaluation right away.
Comparison: Normal Tooth Infection vs. Brain Spread
| Symptom | Local Tooth Infection | Possible Brain Spread |
|---|---|---|
| Tooth pain | Yes | May decrease or persist |
| Facial swelling | Common | Severe, spreading |
| Fever | Mild or none | High, persistent |
| Headache | Mild | Severe, worsening |
| Confusion | No | Yes |
| Seizures | No | Possible |
This table helps clarify how to know if tooth infection spread to brain versus a standard abscess.
How Doctors Diagnose Brain Spread
In U.S. emergency settings, doctors may order:
- CT scan
- MRI
- Blood tests
- Lumbar puncture (if meningitis suspected)
Imaging confirms whether bacteria have formed a brain abscess or caused inflammation.
According to the Centers for Disease Control and Prevention, untreated infections can become systemic, emphasizing the importance of early treatment.
How Fast Can It Happen?
Many people worry about timing. The truth:
- It does not happen overnight in most cases.
- It usually develops after days or weeks of untreated infection.
- Immunocompromised individuals are at higher risk.
However, once symptoms of neurological involvement appear, progression can be rapid.
Emergency Signs That Require 911
Call emergency services immediately if you experience:
- Sudden confusion
- Severe headache with fever
- Trouble breathing
- Seizures
- Fainting
- Swelling closing your airway
Delaying care can lead to permanent brain damage or death.
Treatment Options
Treatment depends on severity.
H3: For Localized Infection
- Antibiotics
- Root canal therapy
- Tooth extraction
- Drainage of abscess
H3: For Brain Involvement
- Hospital admission
- IV antibiotics
- Neurosurgical drainage
- Intensive monitoring
Hospitals follow protocols similar to those recommended by the National Institutes of Health for managing severe infections.
Risk Factors That Increase Spread
Certain conditions raise risk levels:
- Diabetes
- Weakened immune system
- Cancer treatment
- HIV
- Delayed dental care
- Substance abuse
Patients in these categories should never ignore severe dental pain.
Can Antibiotics Alone Prevent Brain Spread?
Antibiotics help, but they are not always enough.
If pus is trapped inside the tooth, antibiotics may temporarily reduce symptoms but won’t eliminate the source. Definitive dental treatment is essential.
This is a critical part of understanding how to know if tooth infection spread to brain—symptoms may temporarily improve before worsening again.
How to Prevent Severe Complications
Prevention is far easier than emergency treatment.
H3: Maintain Routine Dental Visits
Most U.S. dentists recommend checkups every 6 months.
H3: Treat Cavities Early
Small cavities are simple fixes compared to abscesses.
H3: Don’t Ignore Swelling
Facial swelling is never “normal.”
H3: Finish Prescribed Antibiotics
Incomplete courses increase resistance and recurrence risk.
When to See a Dentist vs. ER
See a dentist if you have:
- Localized tooth pain
- Mild swelling
- No fever
Go to the ER if you have:
- Fever over 101°F
- Facial swelling near eye
- Confusion
- Severe headache
- Difficulty breathing
Knowing this difference may save your life.
Real-World Clinical Perspective
In clinical practice, brain complications from dental infections are uncommon but documented. They typically involve delayed treatment, self-medication without dental intervention, or high-risk patients.
Emergency physicians take neurological symptoms seriously when accompanied by dental infection history. Quick imaging and IV antibiotics drastically improve survival rates.
FAQ Section
1. How common is it for a tooth infection to spread to the brain?
It is rare but possible. Most dental infections remain localized if treated promptly. Delays increase risk.
2. Can a tooth infection cause sudden death?
In extremely rare untreated cases, severe sepsis or brain involvement can become fatal. Immediate treatment prevents this outcome.
3. How long can a tooth infection go untreated?
Some infections worsen within days, others over weeks. There is no safe “waiting period.”
4. What does a brain abscess feel like?
Symptoms may include severe headache, fever, confusion, seizures, and vision problems. These are emergency warning signs.
5. Can antibiotics cure a brain infection from a tooth?
Yes, but hospital IV antibiotics and sometimes surgery are required. Oral antibiotics alone are usually insufficient.
Conclusion
Understanding how to know if tooth infection spread to brain can help you respond quickly and appropriately. While brain involvement is rare, the warning signs—high fever, confusion, severe headache, neurological changes—should never be ignored.
Most dental infections are fully treatable when addressed early. Routine dental care, prompt treatment of cavities, and immediate medical evaluation for severe symptoms are the best protections.
If you experience any neurological symptoms alongside a tooth infection, seek emergency care immediately. Acting early can prevent life-threatening complications and ensure a safe recovery.